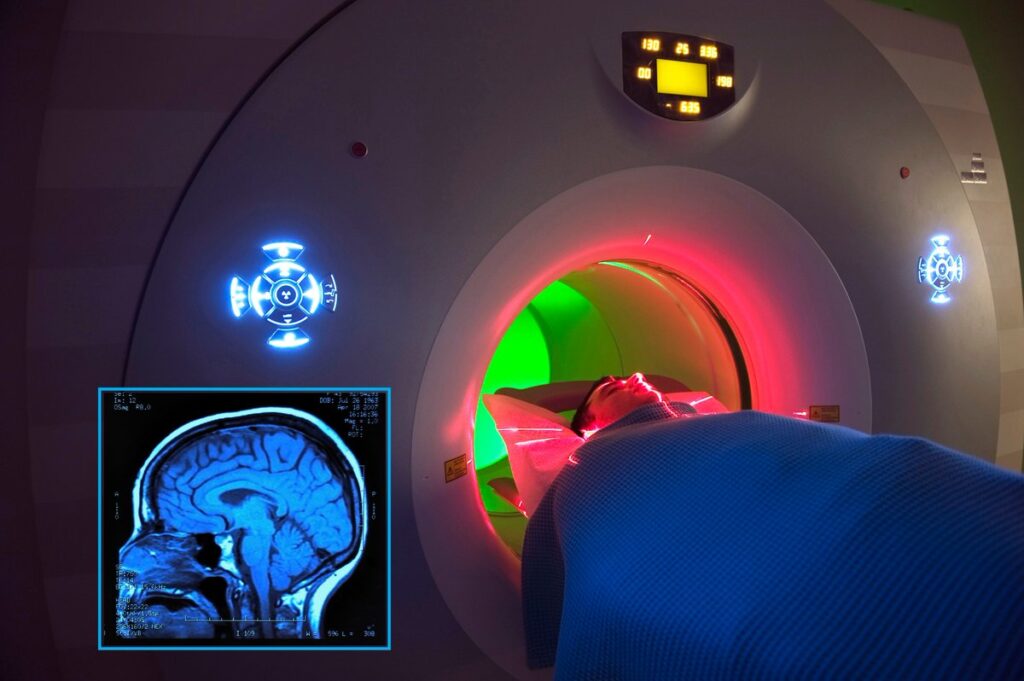
At Big Apple Medical Care, we believe that early diagnosis is the key to effective management of Alzheimer’s disease (AD) and other dementias. Recent advances in MRI (Magnetic Resonance Imaging) and the integration of AI and imaging analytics are transforming what was once possible, enabling detection of Alzheimer’s much earlier, before major cognitive decline has set in. In this article, we explore how MRI is evolving, what the latest research shows, what the challenges are, and what this means for patients, families, and clinicians.
Understanding Alzheimer’s, Dementia, and Why Early Detection Matters
Alzheimer’s disease is a progressive neurodegenerative disorder, the most common cause of dementia. It is characterized by the accumulation of amyloid-β plaques, tau neurofibrillary tangles, synaptic dysfunction, neuronal loss, and brain atrophy, especially in the hippocampus and medial temporal lobes. Dementia, more broadly, refers to a decline in cognitive function severe enough to interfere with daily life; Alzheimer’s is a major subtype.
Early detection is crucial because:
-
Pathological changes begin many years before symptoms appear. Interventions are more effective when applied early.
-
Patients and families can plan care better — medical, social, lifestyle changes.
-
Disease-modifying therapies and clinical trials increasingly target early stages. Structural and functional changes visible in MRI may serve as biomarkers to identify candidates for therapy.
Thus, imaging technology—especially advanced MRI—plays a central role in shifting diagnosis forward in time.
MRI and Related Imaging Techniques: What They Offer
MRI is non-invasive, widely available, and doesn’t expose patients to ionizing radiation, unlike CT or PET. It provides multiple modes to capture both structural and functional/molecular changes:
-
Structural MRI — measures brain volume, cortical thickness, hippocampal size, ventricle enlargement, and patterns of atrophy.
-
Diffusion MRI / Diffusion Tensor Imaging (DTI) — examines the integrity of white matter tracts and connectivity between regions.
-
Functional MRI (fMRI) — detects changes in blood flow (hemodynamics) related to neuronal activity; resting-state fMRI can detect network connectivity disruptions.
-
Advanced techniques / molecular MRI — though more investigational, these techniques aim to detect biochemical changes, microstructural alterations, or may supplement PET imaging.
Recent Advances in MRI for Alzheimer’s & Dementia
Radiomics & Machine Learning for Early Structural Change Detection
Radiomics refers to extracting quantitative features from imaging (texture, shape, intensity, etc.) that are not visible to the naked eye. A recent study using single T1-weighted MRI scans showed that radiomics features could uncover early neuroanatomical changes indicative of Alzheimer’s disease before overt symptoms.
Another line of research (Maity et al.) combined structural MRI and resting-state fMRI, with machine learning models, to distinguish between patients with Mild Cognitive Impairment (MCI) who will convert to Alzheimer’s (“converters”) versus those who will not, with high accuracy.
Deep Learning with Better Slice Selection & Multimodal Fusion
A 2025 study showed that carefully selecting MRI slices (i.e. the most informative cross-sections) when using deep learning models (Vision Transformers, EfficientNet, etc.) can significantly improve diagnostic accuracy, especially for early mild cognitive impairment (EMCI). This method helps focus the model on brain regions showing early signs rather than evaluating all slices, many of which are less informative.
Other work fusing data from T2-weighted MRI, DTI, and structural MRI achieved strong results using advanced neural networks like YOLOv11, distinguishing among stages including early MCI, late MCI, etc.
Brain Age Models & Predicted Age Difference (PAD)
One emerging approach uses MRI to estimate the “biological brain age” vs chronological age. Studies have found that individuals with amnestic Mild Cognitive Impairment (aMCI) often show predicted brain age higher than their actual age; this difference (PAD) correlates with risk of progression to Alzheimer’s.
Integration with Biomarkers, PET and Non-MRI Modalities
While MRI gives structural/anatomical information, combining it with other biomarkers (amyloid-PET, tau-PET, blood tests, CSF markers) improves early detection. PET imaging is more sensitive to specific pathologies (amyloid plaques, tau tangles), but it is more expensive and less widely available. MRI advances can help identify who should undergo more targeted PET imaging.
Imaging for Monitoring Progression and Treatment Responses
MRI is being used longitudinally (i.e. scans over time) to track volume loss, patterns of brain atrophy, and white matter changes. Newer algorithms allow more precise, automated segmentation (e.g. hippocampus, medial temporal lobes) and quantification, enabling clinicians/researchers to see subtle changes over shorter intervals. These metrics can serve as endpoints in clinical trials.
Challenges and Limitations
While the improvements are promising, there are significant challenges:
-
Structural MRI sensitivity is limited in very early stages (preclinical Alzheimer’s). The anatomical changes may not be visible until considerable damage has occurred. Structural MRI alone may not reliably predict who with MCI will progress.
-
Heterogeneity of data: Differences in MRI machines (field strength, vendor), protocols, preprocessing methods lead to variability. Standardization remains a hurdle.
-
Need for large, longitudinal datasets: To validate predictive models, long-term studies with many subjects are needed.
-
Access, cost, and interpretation: High-resolution MRI, advanced analyses, and AI algorithms may not be available everywhere. Also, interpreting complex imaging results can demand specialist radiology/neuroimaging skills.
-
False positives / overdiagnosis risk: Imaging findings alone don’t always translate into clinical Alzheimer’s disease; not all people with amyloid or mild atrophy will develop dementia. Ethical, psychological implications exist in diagnosing disease early when treatments are limited.
What Research & Clinical Practice Suggest: Toward Better Early Diagnosis
Based on recent research and reviews, here are key takeaways for how MRI advances are and can be adopted in clinical practice in Alzheimer’s/dementia care:
-
Multimodal approaches outperform single modalities: Combining structural MRI with DTI, functional MRI, PET, CSF or blood biomarkers gives stronger predictive power.
-
AI / Machine learning + radiomics augment diagnostic accuracy: Deep learning methods, careful slice selection, feature extraction, and predictive modeling help detect subtle changes earlier than visual inspection or standard volumetric measures.
-
Early mild cognitive impairment (EMCI) and prognostication are key targets: Detecting transition from normal cognition to EMCI, and from EMCI to AD, offers opportunities for intervention. MRI advances are allowing better discrimination of these early stages.
-
Standardization and validation: There is movement toward standard protocols for MRI acquisition, image processing, segmentation, automated volumetrics, and AI model training. Large studies / consortia (e.g. ADNI) are helping.
-
Translational potential but cautious implementation: While MRI advances are promising, most new tools are still in research settings. Clinical application requires regulatory, interpretative, ethical, and cost considerations.
What This Means for Patients & Families
For people concerned about dementia, Alzheimer’s, or cognitive decline, recent MRI advances suggest:
-
Earlier conversations with clinicians may be warranted if symptoms are mild (memory lapses, mild confusion, changes in reasoning). Early MRI + cognitive testing + biomarker evaluation increases chances of detecting disease early.
-
Lifestyle interventions (diet, exercise, cognitive stimulation, vascular health) may have more effect if started early. If imaging shows risk or early structural changes, these interventions might slow progression.
-
Participation in clinical trials may be better informed; imaging can help qualify someone for trials of disease‐modifying therapies.
-
Psychological preparation and planning become more possible—if one learns early that changes are occurring, one can plan for care, support, safety, etc.
Big Apple Medical Care’s Approach: Bringing Advances to Practice
At Big Apple Medical Care, we are committed to integrating the latest in MRI imaging and diagnostics into patient care. Our approach includes:
-
Comprehensive imaging protocols: For patients with mild cognitive concerns, we use high-resolution structural MRI with volumetric measures, sometimes diffusion imaging, to assess hippocampal and cortical atrophy, white matter integrity, etc.
-
Collaboration with radiology & neuroscience specialists to interpret advanced imaging features, including radiomics, connectivity, and brain age estimation.
-
AI-assisted tools: Where available and validated, we integrate software tools that help quantify anatomical changes, generate biomarkers, and track progression over time.
-
Multidisciplinary evaluation: Imaging is paired with cognitive testing, biomarker assessments (blood, CSF if appropriate), genetic risk profiling (e.g., APOE), as well as lifestyle risk factor review (vascular risk, sleep, diet).
-
Patient education and shared decision making: We communicate what imaging findings may imply, what they do not imply, and what actionable steps patients can take—lifestyle changes, clinical trial participation, cognitive rehabilitation, etc.
Future Directions in MRI & Dementia Diagnosis
Emerging research suggests several directions that may further shift early detection, diagnosis, and treatment:
-
Ultra-high field MRI (7 Tesla and beyond) may detect microstructural changes earlier, clearer visualization of hippocampal subfields, small vessel disease, etc.
-
Molecular MRI: MRI contrast agents or sequences that target specific molecules (amyloid, tau) are being explored, though PET currently dominates molecular imaging.
-
Longitudinal AI models & predictive risk scores: Combining imaging with genetic, fluid biomarkers, environmental/lifestyle data to generate risk models to forecast who will progress, how fast, and which interventions might help.
-
Wider access and protocol standardization globally: Ensuring that best practices, validated models, and tools are available in diverse populations, with MRI scanners of different strengths, in various healthcare settings.
-
Ethical, regulatory frameworks and patient consent: As early diagnosis becomes possible, considerations around overdiagnosis, privacy of imaging data, counseling before/after imaging findings become crucial.
Conclusion
Recent advances in MRI imaging, AI and deep learning, imaging analysis techniques, and integration with biomarkers are significantly changing how Alzheimer’s disease and other dementias are diagnosed. What once required overt symptoms may now be detectable in EMCI or even preclinical stages. While challenges—sensitivity, standardization, access—remain, the trend is clear: earlier diagnosis, more precise prognostication, and more chances to intervene.
At Big Apple Medical Care, we are committed to leveraging these advances for our patients. We aim to offer imaging and diagnostic strategies that are state of the art, balanced with clinical judgment, ethical care, and patient empowerment. If you or a loved one are concerned about memory changes or cognitive decline, early assessment—including advanced MRI imaging—may offer hope for better outcomes and more options.